What is Radiotherapy?
Radiotherapy, also known as radiation therapy, is a medical treatment that uses high-energy rays to kill cancer cells or slow their growth. It is a common treatment for many types of cancer, including:
– Cancers of the head and neck
– Breast cancer
– Lung cancer
– Colorectal cancer
– Prostate cancer
– Gynecological cancers
– Brain tumors
Radiotherapy in cancer treatment is a burning topic due to sever attack of different types of cancers all over the world.
Types of radiotherapy
There are several types of radiotherapy, including:
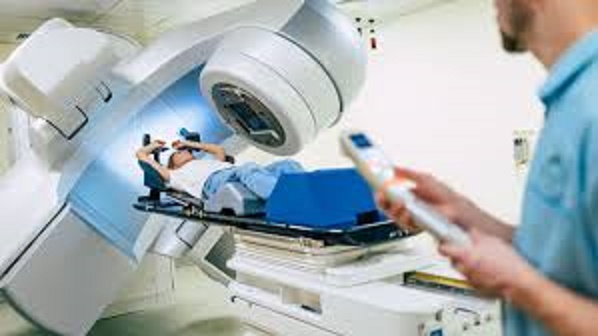
1. External Beam Radiotherapy (EBRT): This is the most common type, where a machine outside the body directs radiation to the tumor site.
2. Internal Radiotherapy (Brachytherapy): Small radioactive implants are placed directly into or near the tumor.
3. Stereotactic Body Radiotherapy (SBRT): High doses of radiation are delivered to small tumors in a few fractions.
4. Intensity-Modulated Radiotherapy (IMRT): Radiation beams are shaped to match the tumor’s shape, reducing damage to surrounding tissue.
5. Image-Guided Radiotherapy (IGRT): Imaging technologies, like X-rays or CT scans, guide the radiation beam to the tumor during treatment.
6. Total Body Irradiation (TBI): The entire body receives low-dose radiation, often before bone marrow transplantation.
7. Total Skin Electron Therapy (TSET): Used to treat skin conditions like mycosis fungoides.
8. Intraoperative Radiotherapy (IORT): Radiotherapy is delivered during surgery, directly to the tumor bed or surrounding tissue.
9. Boron Neutron Capture Therapy (BNCT): A specialized treatment for brain tumors and melanoma.
10. Proton Therapy: Uses protons instead of X-rays to deliver radiation, reducing damage to surrounding tissue.
Each type has its own specific uses and benefits, and the choice of radiotherapy depends on the type and stage of cancer, as well as individual patient needs.
What is cancer?
To understand the role of Radiotherapy in cancer treatment, it is very necessary to study about cancer and types of cancers. Cancer is a group of diseases characterized by the uncontrolled growth and spread of abnormal cells. It occurs when there is a genetic mutation in the DNA of a cell, leading to a breakdown in the normal mechanisms that control cell growth and division.
Cancer cells exhibit several key features, including:
1. Uncontrolled growth: Cancer cells grow and divide uncontrollably, forming masses or tumors.
2. Invasion: Cancer cells invade surrounding tissues and organs.
3. Metastasis: Cancer cells can break away from the primary tumor and spread to other parts of the body through the bloodstream or lymphatic system.
4. Genetic changes: Cancer cells have altered DNA, leading to changes in gene function and expression.
5. Resistance to apoptosis: Cancer cells evade programmed cell death, allowing them to continue growing and dividing.
Types of cancer
There are over 100 types of cancer, which can be broadly classified into several categories:
1. Carcinomas:
– Breast cancer
– Lung cancer
– Colorectal cancer
– Prostate cancer
– Skin cancer (basal cell, squamous cell, melanoma)
– Gynecologic cancers (cervical, ovarian, uterine)
2. Sarcomas:
– Osteosarcoma (bone)
– Soft tissue sarcoma
– Leiomyosarcoma (smooth muscle)
3. Leukemias:
– Acute myeloid leukemia (AML)
– Chronic myeloid leukemia (CML)
– Acute lymphoblastic leukemia (ALL)
– Chronic lymphocytic leukemia (CLL)
4. Lymphomas:
– Hodgkin lymphoma
– Non-Hodgkin lymphoma (NHL)
– Follicular lymphoma
– Diffuse large B-cell lymphoma
5. Brain and spinal cord tumors:
– Glioblastoma
– Medulloblastoma
– Meningioma
– Acoustic neuroma
6. Other types:
– Adenocarcinoma (e.g., pancreatic, thyroid)
– Squamous cell carcinoma (e.g., head and neck, anal)
– Melanoma
– Multiple myeloma
– Thyroid cancer
– Testicular cancer
– Bladder cancer
– Kidney cancer
– Liver cancer
– Stomach cancer
– Esophageal cancer
– Gallbladder cancer
– Bile duct cancer
– Pancreatic cancer
This is not an exhaustive list, and new subtypes of cancer are being identified as research advances. Each type of cancer has unique characteristics, treatments, and survival rates.
Working of radiotherapy technique for cancer treatment
Arguably the most common cancer treatment, radiotherapy, or radiation therapy, uses high-energy radiation to kill cancer cells. Here’s a simplified overview of how it works:
Steps:
1. Simulation: The patient is positioned and imaged to determine the exact location and extent of the tumor.
2. Planning: A radiation oncologist creates a personalized treatment plan, including the type and dose of radiation, number of sessions, and beam angles.
3. Treatment Delivery: The patient is positioned, and radiation is delivered through a machine (linear accelerator or cobalt-60 unit) or internal implants (brachytherapy).
How Radiation Kills Cancer Cells:
1. DNA Damage: Radiation damages the DNA of cancer cells, making it difficult for them to grow and divide.
2. Cell Death: Cancer cells die due to DNA damage, or they may die later due to faulty cell division.
3. Tumor Shrinkage: Radiation can shrink tumors, relieving symptoms and improving quality of life.
Radiation Effects on Normal Cells:
1. Damage: Normal cells can be damaged, but they are more likely to repair themselves than cancer cells.
2. Side Effects: Temporary side effects, like fatigue, skin changes, or hair loss, may occur due to normal cell damage.
Advances in Radiotherapy:
1. Intensity-Modulated Radiation Therapy (IMRT): Precise beam shaping and intensity modulation reduce damage to surrounding tissue.
2. Stereotactic Body Radiotherapy (SBRT): High doses of radiation are delivered to small tumors in few fractions.
3. Image-Guided Radiation Therapy (IGRT): Real-time imaging ensures accurate radiation delivery.
Radiotherapy can be used alone or combined with surgery, chemotherapy, or immunotherapy to achieve optimal outcomes.
Procedure of radiotherapy technique
The procedure of radiotherapy typically involves the following steps:
1. Consultation: The patient meets with a radiation oncologist to discuss treatment options and goals.
2. Simulation: The patient is positioned and imaged (CT, MRI, or PET scans) to determine the exact location and extent of the tumor.
3. Treatment Planning: A personalized treatment plan is created, including:
– Radiation type and dose
– Number of sessions (fractions)
– Beam angles and shapes
– Organs to avoid (critical structures)
4. Immobilization: Devices (molds, masks, or casts) may be used to keep the patient in the correct position during treatment.
5. Treatment Delivery: The patient is positioned, and radiation is delivered through:
– External Beam Radiation Therapy (EBRT): a linear accelerator or cobalt-60 unit
– Internal Radiation Therapy (Brachytherapy): small radioactive sources inserted into or near the tumor
6. Verification: Imaging (X-rays, CT scans, or portal imaging) ensures accurate radiation delivery.
7. Treatment Sessions: The patient receives radiation treatment according to their schedule (daily, weekly, or biweekly).
8. Monitoring: The patient is regularly monitored for:
– Side effects
– Tumor response
– Radiation-induced changes
9. Follow-up: After treatment completion, the patient attends follow-up appointments to assess treatment outcome and manage any long-term effects.
Additional Procedures:
– CT or PET scans: May be performed during treatment to assess tumor response and adjust the treatment plan.
– Tumor localization: Special markers or dyes may be used to help guide radiation delivery.
– Breathing control: Techniques like deep inspiration breath-hold (DIBH) may be used to minimize radiation exposure to critical structures.
Please note that specific procedures may vary depending on the treatment center, radiation oncologist, and individual patient needs.
Precautionary measures for radiotherapy technique
Precautionary measures for radiotherapy technique:
Patient Precautions:
1. Follow instructions: Adhere to radiation oncologist’s advice and treatment schedule.
2. Skin care: Avoid soaps, lotions, and tight clothing that may irritate skin in treatment areas.
3. Hair care: Use gentle shampoos and avoid hair dye or perms during treatment.
4. Nutrition and hydration: Maintain a healthy diet and stay hydrated.
5. Fatigue management: Rest and avoid strenuous activities.
6. Infection control: Practice good hygiene and avoid close contact with people who are sick.
Radiation Safety Precautions:
1. Personal protective equipment (PPE): Wear lead aprons, gloves, and masks as directed.
2. Radiation exposure limits: Ensure radiation doses remain within safe limits.
3. Radiation monitoring: Use dosimeters or badges to track radiation exposure.
4. Shielding: Use lead or concrete shielding to minimize radiation exposure.
5. Emergency procedures: Establish protocols for radiation accidents or spills.
Treatment Room Precautions:
1. Treatment room preparation: Ensure accurate setup and calibration of radiation equipment.
2. Patient positioning: Verify correct patient positioning before treatment.
3. Radiation beam verification: Confirm correct radiation beam alignment and energy.
4. Treatment room access control: Restrict access during treatment to minimize radiation exposure.
Staff Precautions:
1. Training and education: Ensure radiation oncologists, physicists, and technologists receive proper training.
2. Radiation safety protocols: Establish and follow radiation safety guidelines.
3. Personal radiation monitoring: Monitor staff radiation exposure regularly.
4. Quality assurance and quality control: Regularly inspect and maintain radiation equipment.
Other Precautions:
1. Pregnancy and breastfeeding: Take precautions to minimize radiation exposure to the fetus or baby.
2. Implantable devices: Inform your radiation oncologist about pacemakers, implants, or other devices.
3. Metallic objects: Remove metallic objects, like jewelry or glasses, during treatment.
Please note that these precautions may vary depending on the specific radiotherapy technique, treatment center, and individual patient needs.
Visit us:
External Links:
Cancer Patients
Radiotherapy techniques
2 thoughts on “Radiotherapy in cancer treatment”